Retinal Detachment
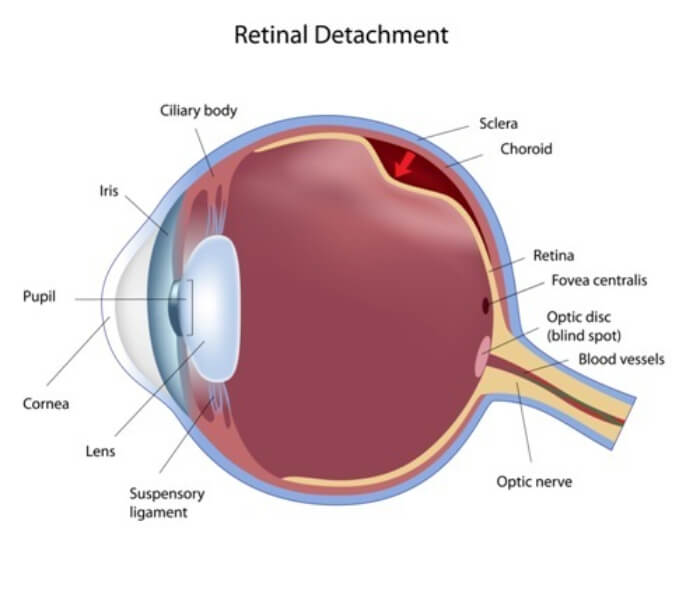
A retinal attachment is an ocular emergency that requires an examination and treatment by a retina specialist. A retinal detachment occurs when the retina pulls away from the choroid which is the part of the eye that supplies nutrients and oxygen to the retina. There are several reasons a retinal detachment can occur. The two most common reasons for retinal detachment are trauma to the head or eye and age of the patient. Patients who have very long eyes (high myopes) are also at a greater risk of having a retinal detachment.
Symptoms of a possible retinal detachment are:
- Sudden increase or appearance of multiple large or small floaters in the vision. Some patients report floaters that appear as “pepper” in the eye.
- Flashes of light that are seen in bright and dim light.
- A veil or curtain in the eye that may appear as a spider web in your vision
- Reduced peripheral vision which can be sudden our gradual.
- Sudden blurred or loss of vision
There are three types of retina detachment: traction, exudative and Rhegmatogenous. All of the types of retina detachments will require treatment and or surgery to repair the detachment.
Certain types of retina detachments and tears can be repaired in the examination or procedure room. Prior to in-office retinal detachment repair, topical or local anesthetic will be placed in the patient’s affected eye to ensure the patient is comfortable during the treatment.
Cryopexy is an in- office procedure in which a cold probe is used to create a scar to seal the retina to the supporting tissue in the back of eye. Cryopexy may, be used in conjunction with Pneumatic Retinopexy to repair a retinal detachment.
Pneumatic Retinopexy, (PR) is a mildly invasive in-office procedure used to repair; superior retina tears, multiple small breaks, and detachments.
This procedure involves injecting a gas or air bubble into in the vitreous. The air bubble will apply pressure to the retina flattening the retina so the retina can adhere to the supporting structure in the back of the eye.
Your retina specialist may ask you to hold your head in a specified position for several days to keep the bubble in the proper place in the back of the eye. Patient cooperation with head positioning is essential for a successful PR treatment. Over time, your body will absorb the bubble, therefor the bubble will not need to be removed.
Your retina physician may not be able to treat your retina tear or detachment in the exam or treatment room and you may need surgery to in the hospital or surgical center repair the detachment.


